Urinary Incontinence Treatments Explained: Medications, Risks, and Options for Men and Women

You may not want to imagine it. Your parent may never mention it. But problems with incontinence can impact men and women well before "old age" and create a nuisance before becoming a much bigger issue.
But when aging begins to limit mobility, incontinence can become a much bigger problem. While many people fail to talk about it, incontinence is more common than you would realize.
Studies show that urinary incontinence affects roughly 25% to 45% of older adults overall, with rates much higher in long-term care settings — up to about 70 percent of nursing home residents experience urinary leakage at some point.
Some surveys find that nearly half of older people report occasional urinary leakage, and others report that more than 50 percent of women and significant proportions of men experience some bladder control issues as they age.
At least one-quarter of women experience some urinary incontinence during their lifetime. You’re absolutely not alone — and talking with your healthcare provider about symptoms can lead to effective treatment options that improve quality of life. — Renee Edwards, M.D., urogynecologist and co-director at the OHSU Center for Women’s Health.
It is common. It is deeply personal. And it can dramatically influence quality of life, staffing demands, and long-term care costs.
Yet most retirement conversations skip over it entirely.
What are the Various Types of Incontinence?
Incontinence is not one condition. It presents in several forms, and some adults may experience symptoms long before they recognize what is happening.
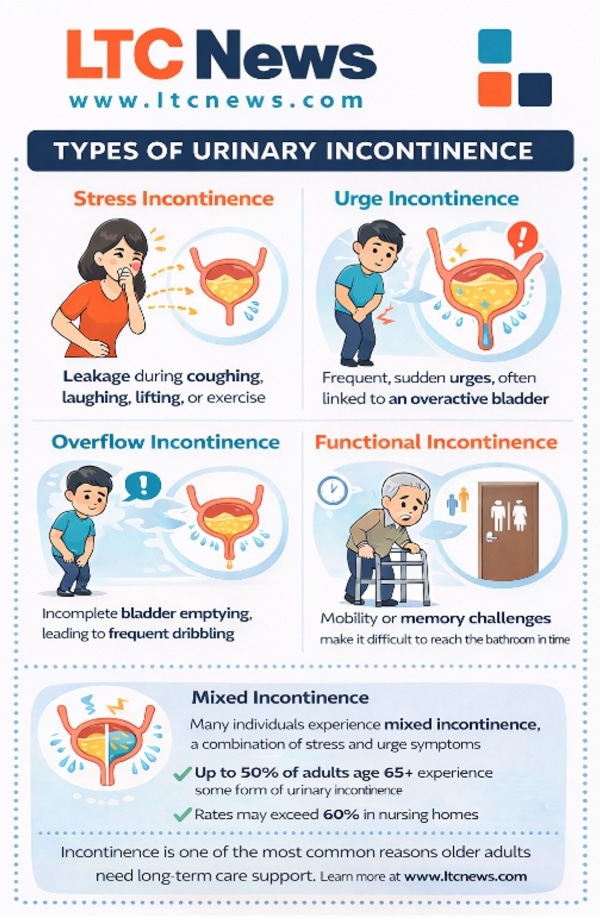
The most common type is stress incontinence, which occurs when physical movement or pressure—such as coughing, laughing, lifting, or exercising—causes urine leakage.
Urge incontinence, often linked to overactive bladder, involves a sudden, intense need to urinate followed by involuntary leakage.
Overflow incontinence happens when the bladder does not empty fully, leading to frequent dribbling.
Functional incontinence occurs when physical or cognitive limitations prevent someone from reaching the bathroom in time, even though bladder function itself may be normal.
Some individuals experience mixed incontinence, a combination of stress and urge symptoms.
Because symptoms may begin subtly—occasional leakage during exercise, waking at night more frequently, or difficulty reaching the restroom in time—many adults dismiss early warning signs as “just aging.”
In reality, incontinence is often manageable, especially when identified early. Recognizing the type and pattern of symptoms allows physicians to recommend targeted treatments, pelvic floor therapy, medication, lifestyle changes, or environmental modifications that may reduce progression and preserve independence.
Fecal incontinence, though less common than urinary incontinence, still affects a meaningful share of older adults. Systematic reviews estimate that about 14 percent of adults age 60 and older experience fecal incontinence, with rates increasing in care settings where residents have higher levels of frailty or mobility impairment.
Today, that silence is beginning to change.
A Common Condition That Few Discuss Openly
Urinary and bowel incontinence increase with age, especially among adults with mobility limitations, stroke history, diabetes, or cognitive decline.
The National Institute on Aging notes that urinary incontinence affects millions of older Americans, particularly women.
In nursing homes, peer-reviewed studies consistently show that more than half of residents experience urinary incontinence, with many facing both urinary and fecal incontinence.
Incontinence is not a niche issue. It is impacting the daily lives of many Americans and others worldwide. It may start as something inconvenient, but it can grow to a problem that adversely impacts your independence and overall quality of life.
It is a central component of long-term care. And as Americans live longer, with more chronic conditions, continence care becomes more complex.
Why Incontinence Is a Health Risk — Not Just a Hygiene Issue
Moisture exposure affects more than comfort.
The National Pressure Injury Advisory Panel identifies excess moisture as a contributing factor in skin breakdown. While incontinence alone does not cause pressure injuries, prolonged moisture, combined with immobility and friction, increases the risk.
Complications may include:
- Skin irritation and incontinence-associated dermatitis
- Greater vulnerability to pressure injuries
- Sleep disruption
- Increased fall risk during nighttime toileting
- Higher caregiver workload
For residents with dementia, embarrassment may reduce social participation. For someone with limited mobility, delayed assistance overnight can accelerate skin compromise.
While this is about dignity, it is also about safety.
How Incontinence Often Begins — And Why It Becomes a Bigger Concern Over Time
You may first notice it in small, almost forgettable ways. A leak when you laugh too hard. A sudden urge during a long drive. Maybe you leak a little on the way to the bathroom at a ball game, or you are waking up once or twice at night when you used to sleep straight through.
In your 40s and 50s, incontinence often starts as a nuisance. Hormonal changes, especially during perimenopause and menopause, can weaken pelvic floor muscles in women.
Men may begin experiencing urinary changes related to prostate enlargement. Weight gain, chronic coughing, high-impact exercise, childbirth history, or certain medications can also contribute. At this stage, many people dismiss symptoms as temporary or “just part of getting older.”
For some, it remains occasional and manageable with lifestyle adjustments or pelvic floor therapy. But as you age, the risk factors increase.
Mobility slows. Arthritis makes it harder to get to the bathroom quickly. Neurological conditions such as Parkinson’s disease or stroke affect bladder signaling. Diabetes can damage nerves involved in bladder control. Cognitive decline may interfere with recognizing or responding to the urge to void.
What started as inconvenient can become disruptive.
Over time, untreated or unmanaged incontinence may begin to affect sleep, social confidence, travel plans, and exercise habits. In advanced stages, especially when combined with limited mobility or dementia, it can become one of the primary reasons a person requires hands-on assistance — and ultimately long-term care.
The progression is not inevitable. Early evaluation and intervention can slow or improve symptoms. But ignoring early warning signs means missing an opportunity to preserve independence.
A leak at 48 may feel embarrassing. At 78, it may influence where you live and who provides your care.
Treatment Options: From Lifestyle Changes to Medical Devices
For millions of middle-aged and older adults, bladder and bowel incontinence are not isolated medical issues but daily realities that affect dignity, comfort, sleep, skin health, and overall quality of life.
The good news is that incontinence is often treatable and, in many cases, manageable with the right combination of medical care, behavioral strategies, and supportive products.
Behavioral and Non-Invasive Treatments
Treatment usually begins conservatively. Physicians often recommend:
- Pelvic floor muscle exercises (Kegels) to strengthen bladder control
- Bladder training, which gradually increases the time between bathroom visits
- Scheduled toileting programs, especially helpful for those living in assisted living and memory care
- Dietary adjustments, such as reducing caffeine or managing fluid timing
- Weight management, which can reduce pressure on the bladder
For fecal incontinence, dietary fiber adjustments and bowel training programs may improve control.
These approaches can be highly effective, especially when symptoms are caught early.
Medications and Medical Interventions
When behavioral strategies are not enough, medical therapies may be considered.
For urinary incontinence, physicians may prescribe:
- Medications to calm overactive bladder muscles
- Topical estrogen therapy for postmenopausal women
- Beta-3 adrenergic agonists or anticholinergics (when appropriate and medically safe)
Men with prostate-related urinary symptoms may benefit from medications that relax or shrink prostate tissue.
In more persistent cases, additional options may include:
- Nerve stimulation therapies
- Botox injections into the bladder muscle
- Minimally invasive procedures or surgical interventions
- Bulking agents to improve urethral closure
Treatment decisions depend on the type of incontinence, overall health, medication interactions, and mobility level. Evaluation by a primary care physician, urologist, or urogynecologist is often the first step.

While medications can significantly improve symptoms, they are not one-size-fits-all. Always review potential side effects, especially for older adults where cognitive risks and fall concerns exist, before starting treatment.
Absorbent Products and Skin Protection
For many older adults, especially those with mobility limitations or cognitive decline, protective products remain an essential part of care.
These include:
- Absorbent briefs and protective undergarments
- Bed pads and chair protectors
- Barrier creams to prevent skin irritation
- Cleansing products formulated for fragile skin
Moisture management is critical. Prolonged exposure to urine or stool increases the risk of skin irritation and breakdown, particularly in residents with limited mobility.
Technology-Assisted Monitoring
As senior living communities face rising resident acuity and staffing pressures, some providers are turning to monitoring technology to improve responsiveness.
In January 2026, Kentucky Gov. Andy Beshear (D-KY) attended a ribbon-cutting ceremony in Louisville to recognize Wicked Technologies' expansion. The governor issued a proclamation designating Jan. 28 as “Wicked Works Day” to highlight healthcare innovation.
The company’s flagship product, the Wicked Smart Pad®, is an FDA-regulated, washable, reusable medical device designed to detect moisture events and notify caregivers through connected monitoring systems. The goal is to provide care teams with greater visibility into incontinence-related moisture events that might otherwise go unnoticed between scheduled rounds.

Technology like this does not replace hands-on care or clinical judgment. Instead, it functions as an adjunct tool that may help reduce prolonged moisture exposure, support documentation, and improve workflow consistency.
A Comprehensive Approach
There is no single solution for incontinence. Effective management often requires a layered approach:
- Early medical evaluation
- Targeted treatment based on type
- Structured toileting programs
- Protective products
- Skin monitoring
- In some settings, technology-assisted awareness tools
When addressed early, incontinence may remain manageable and less disruptive. When ignored, it can become a primary driver of hands-on care needs and, in some cases, transition to assisted living or nursing home placement.
Help for the Growing Caregiving Strain
Incontinence management does not happen in isolation. It adds to the caregiver workload at a time when family and professional caregivers are already stretched.
According to LTC News reporting based on national data, 63 million Americans now provide unpaid care, a 45% increase since 2015. Many family caregivers juggle careers, children, and aging parents simultaneously. These family caregivers are n ot trained or prepared for this type of stress and responsibility. Caring for a loved one is hard enough without dealing with bathroom issues and incontinence.
Professional in-home caregivers are trained and prepared, but health insurance and Medicare will not pay for this type of extended care. Unless a loved one has a Long-Term Care Insurance policy, family members are often forced to step in, or they pay for professional caregivers.
In senior living communities, staff must balance continence checks with medication passes, fall prevention, mobility assistance, and documentation.
Traditional workflows rely on:
- Scheduled rounding
- Manual checks
- Resident self-reporting
- Visual observation
But incontinence events are unpredictable. They often occur overnight or between rounds. Even strong teams face visibility limitations.
The Financial Reality Families Often Miss
Incontinence is rarely discussed between friends and family and certainly not in retirement planning. But it can directly influence long-term care needs.
Assisted living and nursing home residents often require hands-on continence support multiple times per day. In-home care plans frequently include toileting assistance several days per week.
According to the LTC News comprehensive survey of long-term care costs nationwide, the cost of extended care services continues to rise. It can be very expensive depending on where you live.
- Assisted living base costs commonly range from $4,500 to $6,000 per month in many regions, and surcharges can add $2,000 or more on top.
- Skilled nursing care can exceed $8,000 to $10,000 or more per month.
- In-home care often ranges from $25 to $40 per hour, depending on location.
Medicare does not pay for ongoing custodial long-term care. It covers up to 100 days of skilled nursing care following a qualifying hospital stay, provided medical criteria are met.
Traditional health insurance also does not cover extended assistance with activities of daily living, including toileting support.
That leaves families paying out of pocket unless they qualify for Medicaid, which has strict income and asset limits.
Long-Term Care Insurance is designed specifically to help cover these extended care costs, including in-home care, assisted living, and nursing home services. Benefits can help protect retirement assets and reduce the burden on adult children.
For many people, long-term care is synonymous with being in a nursing home or losing nearly all mobility. While that can happen, most long-term care actually involves help with everyday activities, support with mobility, and supervision due to memory impairment.
Incontinence is one of the most overlooked activities of daily living. People often dismiss it as a minor inconvenience, yet it can significantly affect dignity, comfort, and overall quality of life.
Ignoring incontinence in planning discussions means overlooking one of the most common and realistic drivers of hands-on care needs as you age.
Take Advantage of the Available Treatment
A wide range of medications, treatments, and supportive products can help those impacted by incontinence maintain comfort and independence. However, you must talk to your doctor about the problem, sooner rather than later. Don't be embarrassed about the issue.
Depending on the type and cause, your doctor may recommend bladder-calming medications, topical hormone therapy for postmenopausal women, prostate-related treatments for men, pelvic floor physical therapy, or minimally invasive procedures such as nerve stimulation or bladder injections.
Behavioral strategies like bladder training and scheduled toileting can also significantly reduce episodes.
For daily management, absorbent undergarments, protective bedding, skin barrier creams, and moisture-wicking products help prevent irritation and protect fragile skin. Devices such as the Wicked Smart Pad® represent part of this shift toward data-informed continence management. By detecting moisture events and transmitting alerts, these systems support caregiver workflows rather than replace clinical judgment.
When used together under medical guidance, these options can reduce accidents, improve sleep, preserve dignity, and support a better overall quality of life.
The message is simple: Effective incontinence management is not about containment. It is about responsiveness, consistency, and respect.
What You Should Ask Before Choosing a Long-Term Care Provider
If you are evaluating potential long-term care options for an older family member, be sure to assess how they handle incontinence.
You can narrow down caregivers and long-term care facilities by using the LTC News Caregiver Directory. Then, schedule a time to ask important questions.
- How is continence care managed overnight?
- How often are rounds conducted?
- How is skin integrity documented?
- What is the staff-to-resident ratio?
- Are technology-assisted monitoring tools used?
Transparency matters. So does preparation.
If more than half of Americans who meet the federal definition of long-term services and supports will need care during their lifetime, why leave one of the most common care realities out of the conversation?
Use the LTC News Cost of Care Calculator to see what the average extended care costs in your area. If a loved one has a Long-Term Care Insurance policy, be sure to use the benefits. Get help with processing the insurance claim, as LTC News, along with Amada Senior Care, will help you process a claim for any Long-Term Care Insurance policy without the cost of obligation. They can also evaluate your loved one's situation and make appropriate care recommendations — File a Long-Term Care Insurance Claim.
Explore Long-Term Care Insurance options for yourself before your health changes, limiting eligibility and increasing the cost.


