A Simple Blood Test May Predict When Alzheimer’s Symptoms Begin

About This Article
A new study published in Nature Medicine shows that a plasma biomarker “clock model” can estimate Alzheimer’s symptom onset within three to four years. Here’s what that means for you and your future planning.

James Kelly
LTC News staff writer specializing in long-term care and aging.
You may have watched a parent slowly decline. You may worry about your own memory. And like many adults over 40, you probably wonder: If Alzheimer’s is coming, how early would I know?
Researchers now say a simple blood test may help answer not only whether Alzheimer’s disease is developing, but also approximately when symptoms might begin.
A new study published February 19th in Nature Medicine, led by scientists at Washington University School of Medicine in collaboration with the Foundation for the National Institutes of Health Biomarkers Consortium, suggests that a single blood measurement of a protein called p-tau217 can estimate symptom onset within about 3 to 4 years.
Researchers emphasize the tool is designed for research use—not personal medical forecasting. But its implications for Alzheimer’s trials, early intervention, and long-term care planning are significant.
What Is p-Tau217?
Alzheimer’s disease develops silently for years, often decades, before symptoms appear.
During that time:
- Amyloid plaques accumulate in the brain
- Tau proteins become abnormally phosphorylated
- Nerve cells gradually lose function
Traditionally, confirming these changes required PET scans or spinal fluid testing. Those methods are accurate but expensive and limited in availability.
The new study focuses on plasma p-tau217, a blood-based biomarker strongly linked to both amyloid and tau pathology in the brain.
In simple terms:
- Higher p-tau217 levels in blood reflect Alzheimer’s-related brain changes
- Levels tend to rise in a measurable pattern before symptoms begin
- That pattern can be modeled over time
How the “Clock Model” Works
Researchers analyzed blood samples from more than 600 adults ages 62 to 78 who were initially cognitively normal. Participants were followed for up to 10 years.
Using repeated measurements of plasma p-tau217, the team created statistical “clock models” that estimate when a person crosses a biomarker threshold associated with Alzheimer’s pathology. From that estimated point, researchers calculated the expected time to symptom onset.
The result: The model predicted symptom onset with a median margin of error of approximately three to four years.
“This study demonstrates that blood tests can potentially predict not only whether individuals are likely to develop Alzheimer’s symptoms, but also provide an estimate of when symptoms may begin.” — Suzanne Schindler, MD, PhD, associate professor of neurology at Washington University School of Medicine and senior author of the study.
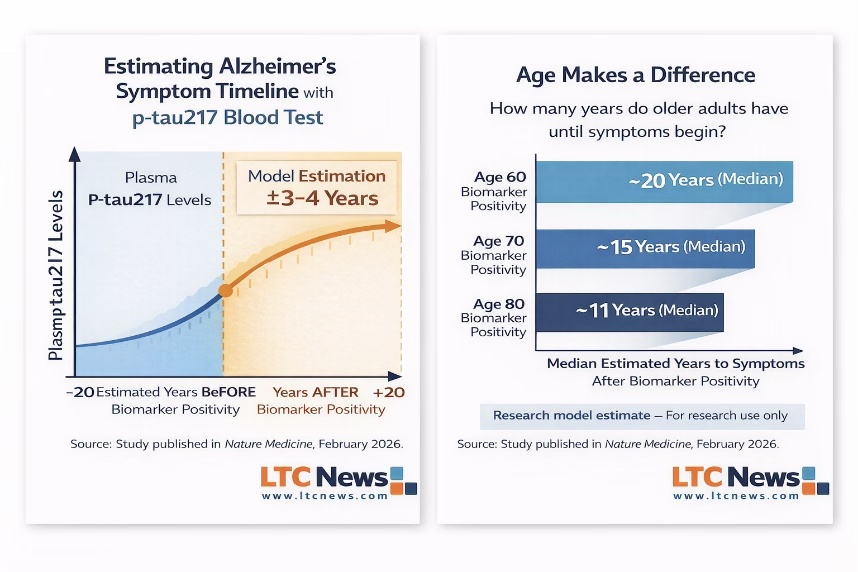
Age Changes the Timeline
One of the study’s most important findings: age matters. Participants who reached elevated p-tau217 levels at younger ages tended to have a longer time to symptom onset. Older individuals progressed more quickly once biomarker levels rose.
In other words, a 60-year-old and an 80-year-old with similar p-tau217 levels may face very different timelines.
This aligns with what neurologists have long observed: the aging brain has less resilience and often accumulates additional pathologies, including vascular disease.
Why This Matters for Clinical Trials
The clock model may be particularly useful for prevention trials. Alzheimer’s trials often struggle because many participants do not develop symptoms during the study period.
If researchers can better identify individuals who are likely to convert to symptomatic Alzheimer’s within three to five years, trials could:
- Become shorter
- Require fewer participants
- Reduce overall cost
- Improve statistical power
“With advances in Alzheimer’s blood-based diagnostics, the field is moving closer to earlier detection and more accessible, precise treatments.” — Alessio Travaglia, PhD, director of translational science, neuroscience and rare diseases at the Foundation for the National Institutes of Health.
The study also introduced a web-based research tool that allows scientists to visualize how p-tau217 levels change over time in relation to symptoms.
Researchers stress that both biomarker testing in asymptomatic individuals and the use of the modeling tool should remain limited to research settings.
What This Means for You
Right now, this blood test model is not intended for routine screening of people without symptoms.
Major medical groups, including the Alzheimer's Association, caution against broad biomarker testing in cognitively normal adults outside research settings due to limited actionable guidance and ethical considerations.
However, the direction of science is clear: blood-based Alzheimer’s diagnostics are becoming more accurate, accessible, and informative.
And that has long-term implications.
Alzheimer’s and Long-Term Care Planning
Alzheimer’s disease remains one of the leading drivers of long-term care needs. According to the U.S. Department of Health and Human Services, 56 percent of Americans who reach age 65 will require long-term services and supports that meet the federal definition—help with two or more activities of daily living or significant cognitive impairment.
Cognitive decline often leads to:
- In-home caregiving
- Assisted living
- Memory care
- Skilled nursing care
People require extended care for several reasons, including chronic illness, mobility difficulties, dementia, and frailty due to aging.
Most long-term care is not covered by health insurance or Medicare. Unless you have Long-Term Care Insurance—or qualify for Medicaid after exhausting much of your savings—the financial burden can fall directly on you and your family, often creating significant emotional and economic strain.
Costs vary widely by location and level of care. You can explore current local costs using the LTC News Cost of Care Calculator, which surveys providers nationwide.
While this new blood test cannot yet tell you exactly when symptoms would begin, earlier detection research underscores an important reality:
Planning before a diagnosis preserves more options.
Once cognitive impairment is documented, eligibility for Long-Term Care Insurance or certain financial planning tools may be limited.
Because of medical underwriting, the availability of LTC Insurance requires reasonably good health when you apply. That is one of several reasons experts suggest obtaining coverage before retirement. Most people who acquire an LTC policy are between 47 and 67.
Important Limitations
Researchers acknowledge several limitations:
- The model applies only within specific biomarker ranges.
- It was primarily developed for non-Hispanic White populations.
- Coexisting brain diseases can influence symptom timing.
- The prediction window still carries a three-to-four-year margin of error.
The authors explicitly discourage individuals from using these models to estimate personal symptom onset outside research settings.
The Bigger Picture
For decades, Alzheimer’s research focused on diagnosing the disease after symptoms appeared. This study represents a shift toward modeling the disease timeline before noticeable decline.
If refined and validated further, plasma biomarker clocks could help:
- Identify high-risk individuals for prevention trials
- Guide earlier therapeutic intervention
- Inform more timely family discussions
- Shape future standards of care
But science is still evolving.
A Question Worth Asking
If you knew your risk window was narrowing, would you change your retirement timeline? Your housing decisions? Your insurance coverage?
You cannot control whether Alzheimer’s research advances. You can control whether you prepare while it does.
Caring for a Loved One with Alzheimer's
When someone you love develops Alzheimer’s disease, life changes gradually—and then all at once. What begins as small memory lapses can evolve into increasing supervision, hands-on assistance, and eventually full-time care.
At first, caregiving may involve reminders, transportation to appointments, and help managing medications or finances.
Over time, many families face more intensive responsibilities:
- Assisting with bathing, dressing, and toileting
- Managing wandering or safety concerns
- Handling behavioral changes or agitation
- Coordinating medical visits and therapy
- Providing constant supervision
The emotional toll can be just as heavy as the physical demands. Watching a spouse or parent lose independence is heartbreaking. Caregivers often report high levels of stress, sleep disruption, and financial strain.
According to the latest data reported by LTC News, 63 million Americans are now providing unpaid care, a 45% increase since 2015. Alzheimer’s and other dementias account for a significant share of that caregiving burden. Memory care can be exceptionally difficult for loved ones.
At some point, care needs may exceed what a family can safely provide at home. Options may include:
- In-home professional caregiving
- Adult day programs
- Assisted living with memory care
- Skilled nursing care
Finding quality extended care is essential to maintaining the best possible quality of life for a loved one.
Use the LTC News Caregiver Directory to search for quality extended care services: Find memory care facilities near you.
This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for personalized medical guidance.