How Immigration Policy Is Deepening the Healthcare Worker Shortage

About This Article
Healthcare workforce shortages may intensify amid federal policy shifts. Immigration restrictions are deepening U.S. healthcare worker shortages, impacting hospitals, long-term care, and access to care nationwide.

Beata Dejlitko McCann
A child of Polish immigrants and a licensed Illinois CPA, is a nationally known immigration attorney focused exclusively on business-based immigration, with deep experience in employment- and investor-based matters.
Table of Contents
- Aging Population Drives Rising Demand for Care - Critical Staffing Challenges Ahead
- Immigrants Play a Key Role in Healthcare Delivery
- Economic Contributions of Immigrant Healthcare Workers
- Healthcare Job Growth Highlights Sector Dependence
- Immigration Enforcement Changes Create New Barriers
- Visa Policy Changes Increase Hiring Costs and Complexity
- Administrative Hurdles Slow Recruitment of Foreign Workers
- Country-Based Restrictions Disrupt Workforce Pipeline
- Work Authorization Changes Add Workforce Instability
- Rural Communities Face Disproportionate Impact
- Nursing Shortages Add to Systemwide Strain
- Home Care Sector Particularly Vulnerable
- Policy Changes Affect Patient Access and Coverage
- Healthcare System Feels Ripple Effects of Policy Decisions
- Staffing Challenges Threaten Future Healthcare Access
- Quick Takeaways
The Trump administration’s immigration crackdown is hitting at a bad time for American healthcare. Hospitals, nursing homes, home care agencies, and long-term care providers were already struggling to hire enough physicians, nurses, aides, and support staff. Now, a tougher enforcement climate and a growing list of immigration restrictions are making that problem worse.
For older adults and the families who rely on home care, assisted living, nursing homes, and local hospitals, the consequences are real. They show up in longer wait times, staffing gaps, reduced access to care, and more pressure on an already strained system.
The labor shortage in healthcare is increasing. Federal projections show the United States could face a shortfall of 141,160 full-time-equivalent physicians by 2038. Nursing shortages are also expected to continue, including projected shortages of 108,960 registered nurses and 245,950 licensed practical nurses by the same year. In long-term services and supports (LTSS), demand is expected to rise 40 percent between 2023 and 2038, growing from 2.35 million workers to 3.29 million.
Aging Population Drives Rising Demand for Care - Critical Staffing Challenges Ahead
This is the backdrop. The population is aging, demand for care is rising, and the workforce is already under pressure.
Long-term care is one of the clearest examples. It depends heavily on workers who are difficult to recruit and even harder to replace. HRSA projects that by 2038, demand for home health aides will increase by 36 percent, demand for nursing assistants by 44 percent, and demand for personal care aides by 38 percent. Direct care workers are expected to make up about two-thirds of the LTSS workforce by then. Demand for nurses in long-term care settings is also projected to rise sharply.
As such, the problem is not limited to doctors. The country also needs the workers who help older adults bathe, dress, eat, recover at home, and avoid unnecessary hospitalizations. Those roles are essential, and there are not enough people to fill them.
Immigrants Play a Key Role in Healthcare Delivery
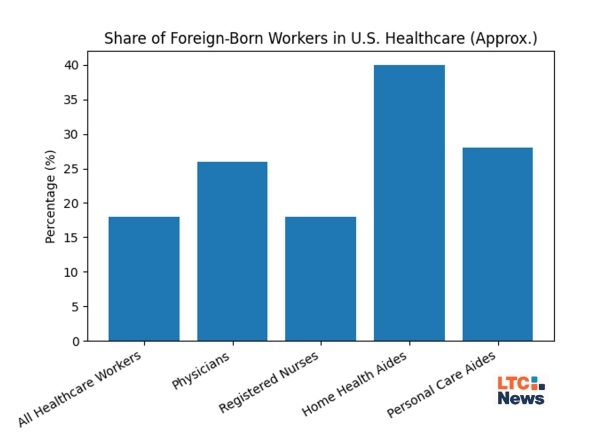
Immigrants are a major part of that workforce. A widely cited review found that immigrants make up 28 percent of physicians and surgeons and 37.9 percent of home health aides, despite accounting for just 13.6 percent of the overall U.S. population. Data from the Migration Policy Institute show that immigrants play an especially important role in healthcare occupations and geographic areas where shortages are already severe.
More recent reporting found that foreign-born workers made up about 18 percent of the healthcare workforce in 2023, including substantial numbers of noncitizen physicians, registered nurses, and home health or personal care aides.
Economic Contributions of Immigrant Healthcare Workers
Immigrants also contribute more to the healthcare system than many political talking points suggest. One report found that immigrants paid $51 billion more into Medicare than they used in Medicare-funded services between 2012 and 2018. On average, immigrants are younger, healthier, and more likely to be working age than the U.S.-born population.
Many noncitizens are also ineligible for a wide range of federally funded health benefits. In practical terms, that means many immigrant workers are helping support the financing of care, including care for older Americans who rely on Medicare.
Healthcare Job Growth Highlights Sector Dependence
This is all happening while healthcare has become one of the country’s biggest drivers of job growth. KFF Health News reported that healthcare accounted for nearly half of all U.S. job growth in the first eight months of 2025. It also noted that home health employment increased by nearly 300,000 workers between August 2019 and August 2025, reaching roughly 1.82 million workers. That growth reflects real need, especially in home-based care and aging-related services. It also means the sector is especially vulnerable to immigration disruptions.
Immigration Enforcement Changes Create New Barriers
Since returning to office, President Trump and his administration have taken a far more aggressive immigration approach. Supporters describe that as restoring order and strengthening enforcement. In healthcare, the practical result is more friction. There is more uncertainty for employers, more difficulty for foreign workers and trainees, more delays in visa processing, and more cost for organizations that are already struggling to hire.
One of the first major changes was the rescission of the “protected areas” policy. DHS and ICE no longer generally treat hospitals, schools, and houses of worship as places to avoid for immigration enforcement. That does not mean agents are present in every hospital, but it does remove a layer of assurance that once mattered to patients, families, and healthcare institutions. Past research and prior policy experience have already shown that immigration-related fear can discourage people from seeking care. In healthcare, delayed care usually means people show up sicker, later, and in more expensive settings.
Visa Policy Changes Increase Hiring Costs and Complexity
The administration has also made legal employment-based immigration more expensive and more difficult. In September 2025, a presidential proclamation imposed a $100,000 payment requirement for certain new H-1B petitions. Then, in a final rule published in late December 2025 and effective in February 2026, DHS replaced the standard H-1B cap lottery with a weighted selection process favoring higher-wage registrations.
For healthcare employers, that creates obvious problems. Large urban systems may be able to absorb higher recruitment costs or compete on salary. Smaller employers often cannot. Rural hospitals, community providers, and long-term care facilities tend to have less financial flexibility, even when their need is urgent. HRSA projects that by 2038, nonmetro areas will have only 42 percent of the physician supply they need, compared with 95 percent in metro areas. A wage-weighted visa selection system and $100,000 visa fees do little to help communities already struggling the most.
Administrative Hurdles Slow Recruitment of Foreign Workers
The visa process itself has also become harder to manage. The State Department initially expanded interview waivers early in 2025, then later narrowed them significantly. By September and October 2025, most non-immigrant visa applicants will once again generally need in-person interviews, with only limited exceptions. The government also moved toward requiring applicants to schedule in their country of nationality or residence, reducing the flexibility many once had to use third-country consulates with shorter wait times. On top of that, the State Department expanded social media screening and instructed certain applicants to make their online presence publicly viewable.
Taken together, those changes create greater delays, higher costs, and greater unpredictability for employers trying to recruit physicians, nurses, researchers, trainees, and other healthcare workers from abroad.
Country-Based Restrictions Disrupt Workforce Pipeline
Country-based restrictions have added another layer of disruption. In June 2025, the administration suspended or partially suspended visa issuance and entry for nationals of 19 countries. That policy expanded to 39 countries effective January 1, 2026. Separately, the State Department announced a pause on the issuance of immigrant visas for nationals of 75 countries, effective January 21, 2026. In healthcare, those restrictions have immediate consequences.

Some physicians, nurses, researchers, residents, and family members can no longer arrive on schedule. Some cannot come at all. When staffing is already thin, even one delayed arrival can affect schedules, call coverage, patient access, and admissions.
Work Authorization Changes Add Workforce Instability
Workers already in the United States are also facing greater instability. DHS ended automatic extensions of employment authorization for many renewal applicants effective October 30, 2025. That increases the risk that workers waiting for renewals will face gaps in their work authorization if adjudications are delayed. In healthcare settings where turnover is high and schedules are hard to cover, that becomes a real operational problem very quickly.
Rural Communities Face Disproportionate Impact
The pressure is especially acute in rural America. HRSA projects a 58 percent physician shortage in nonmetro areas by 2038, compared with a 5 percent shortage in metro areas. Several specialties that older adults rely on heavily, including family medicine, geriatrics, and hospital medicine, are already expected to remain tight.
In many rural communities, those physicians are the backbone of care. They manage chronic disease, coordinate treatment, and serve patients with complicated needs. When international recruitment becomes harder, the damage is not evenly spread. It lands hardest in the places that already had the fewest options.
Nursing Shortages Add to Systemwide Strain
Nursing tells the same story. HRSA projects that registered nurse shortages will continue nationally through 2038, with worse gaps in nonmetro areas. It also projects that the LPN supply will meet only 70 percent of demand by 2038. In long-term care, those shortages are not interchangeable. RNs, LPNs, aides, and personal care workers each do different work. When one category is short, the strain shifts to everyone else. Overtime increases, burnout gets worse, turnover follows, and family caregivers are left trying to close the gap.
Home Care Sector Particularly Vulnerable
Home care and long-term care are particularly vulnerable because they rely so heavily on direct care labor and often operate on narrow margins. HRSA projects that by 2038, demand for home health aides will reach 526,340, demand for nursing assistants will reach 881,950, and demand for personal care aides will reach 770,880. Immigrants already make up a disproportionately large share of these roles. So when immigration policy slows the arrival of new workers, makes existing workers more fearful, or creates more work authorization problems, providers have very few good alternatives. Agencies compete for the same small labor pool, families struggle to find help, and more caregiving responsibilities shift back onto relatives at home.
Policy Changes Affect Patient Access and Coverage
The effects are not limited to staffing. The administration’s immigration agenda is also affecting healthcare from the patient side. CMS finalized a rule removing DACA recipients from the definition of “lawfully present” for ACA marketplace and Basic Health Program eligibility. HHS broadened its interpretation of “federal public benefits” across several health-related programs (although parts of that policy have been blocked in plaintiff states, and litigation is ongoing). CMS also launched a nationwide Medicaid and CHIP eligibility-enforcement initiative focused on citizenship and satisfactory immigration status.
These are not hiring rules, but they still affect providers. When eligibility becomes more restrictive, and fear grows around using healthcare services, safety-net providers often end up dealing with the fallout. That can mean delayed care, more administrative burden, more uncompensated treatment, and less stable reimbursement.
Healthcare System Feels Ripple Effects of Policy Decisions
Healthcare does not operate in a vacuum. Staffing, patient access, reimbursement, and public trust all affect one another. If a rural hospital cannot recruit a physician, nearby patients and facilities feel it. If a home care agency cannot keep enough aides on staff, family caregivers feel it. If immigrant families avoid care because they are afraid or confused, conditions often worsen before anyone gets treatment.
Immigration policy and healthcare policy are closely connected, whether policymakers admit it or not.
Staffing Challenges Threaten Future Healthcare Access
People can disagree about border security and immigration enforcement. But the staffing reality in healthcare is hard to argue with. The country needs more physicians, more nurses, more direct care workers, and more home-based support, especially as the population gets older and more people want care closer to home. At the same time, the Trump administration is raising hiring costs, adding visa barriers, increasing enforcement pressure, and restricting entry for workers from dozens of countries.
In a healthcare system that is already short on people, those choices make it harder to staff facilities, harder to expand care, and harder to build the workforce the country actually needs.
Quick Takeaways
- Healthcare worker shortages are worsening. The U.S. is projected to face major shortfalls in physicians, nurses, and long-term care workers by 2038.
- Immigrants are essential to care delivery. They make up a significant share of doctors, nurses, and especially home health aides who support older adults.
- Immigration policy changes are adding pressure. Higher visa costs, stricter rules, and delays are making it harder for healthcare providers to hire needed staff.
- Rural communities face the biggest risk. Nonmetro areas are expected to experience the most severe shortages, limiting access to care.
- Long-term care demand is rising fast. An aging population will increase the need for home care aides, nursing assistants, and personal care workers.
- Families may feel the impact first. Staffing shortages can shift more caregiving responsibilities onto spouses and adult children.
- Patient access to care could decline. Fewer workers may lead to longer wait times, delayed treatments, and reduced services.
- Immigrants support the healthcare system financially. Many contribute more to programs like Medicare than they receive in benefits.
- Delays in care can worsen health outcomes. Fear or confusion around immigration enforcement may cause some patients to avoid seeking care until conditions become serious.
- Policy and healthcare are closely connected. Immigration decisions directly affect staffing, access, and the overall stability of the U.S. healthcare system.
Frequently Asked Questions
How do visa changes affect healthcare hiring?
New policies, including higher visa fees and wage-based selection systems, increase hiring costs and limit access to international talent. Smaller healthcare providers and rural facilities are especially impacted.
Why are immigrants important to the healthcare system?
Immigrants play a critical role in U.S. healthcare. They make up about 28% of physicians and nearly 38% of home health aides, helping fill essential roles that are already experiencing shortages.
What happens when patients delay care due to immigration concerns?
Fear or uncertainty around immigration enforcement can cause individuals to delay seeking care. This often results in more serious health issues and higher costs when treatment is finally received.
What role do immigrants play in long-term care?
Immigrants are heavily represented in long-term care roles such as home health aides and personal care workers. These positions are essential for helping older adults with daily activities and maintaining independence.
How do immigration restrictions impact patient care?
When healthcare facilities cannot hire enough staff, patients may experience:
- Longer wait times
- Reduced access to care
- Delayed treatments
- Increased strain on existing providers
Are rural communities more affected by healthcare worker shortages?
Yes. Rural areas are expected to face much larger shortages, with projections showing they may have only 42% of the physician supply needed by 2038.
How does immigration policy affect long-term care services?
Restrictions on immigration can worsen staffing shortages in long-term care, leading to:
- Fewer available caregivers
- Increased burden on family members
- Reduced availability of home-based care services
How is demand for long-term care expected to change?
Demand for long-term services and supports is projected to increase by about 40% between 2023 and 2038, driven largely by the aging population.
How is immigration policy affecting the U.S. healthcare workforce?
Immigration policy changes are making it harder for healthcare employers to recruit and retain workers. Increased visa restrictions, higher costs, and processing delays are reducing the number of foreign-born physicians, nurses, and caregivers entering the workforce.
What does this mean for families and caregivers?
As staffing shortages worsen, families may need to take on more caregiving responsibilities. This can lead to emotional stress, financial strain, and reduced access to professional care.
Are immigrants a financial burden on the healthcare system?
Research shows immigrants often contribute more to programs like Medicare than they use. Between 2012 and 2018, immigrants paid $51 billion more into Medicare than they received in benefits.
What healthcare worker shortages are expected in the future?
Federal projections show significant shortages by 2038, including:
- Over 141,000 physicians
- Nearly 109,000 registered nurses
- About 246,000 licensed practical nurses
Demand for long-term care workers is also expected to grow sharply.